2Department of Nuclear Medicine, İstanbul University-Cerrahpaşa, Cerrahpaşa Faculty of Medicine, İstanbul-Türkiye DOI : 10.5505/tjo.2022.3385
Summary
OBJECTIVEThe aim of this study is to calculate embryo/fetal doses in pregnant women who received 99mTc-labeled radiopharmaceuticals for SPECT/CT scan.
METHODS
Embryo/fetal doses were estimated for 74 pregnant women underwent SPECT/CT scan from different
regions of Turkey. OLINDA/EXM package program was used for radiation dose calculation from internal
emitters, while CT dose was calculated from modified soft-tissue CT dose index.
RESULTS
The highest embryo/fetal dose was found in 99mTc- methoxy isobutyl isonitrile (MIBI) myocardial perfusion
scintigraphy (MPS) as (8.88+5.55=14.43 mGy) from both distinct modes (stress and rest imaging).
The embryo/fetal dose from MPS slightly increased to 15.63 mGy with the CT dose contribution.
Whereas, 99mTc- dimercaptosuccinic acid (DMSA) static renal scintigraphy recorded the lowest embryo/
fetal dose among the other diagnostic procedures (mean 1.06 mGy).
CONCLUSION
The embryo/fetal doses increased with simultaneous CT scans in nuclear medicine modalities. Questioning
pregnancy before scintigraphy is obligatory the first-line strategy to avoid radiation exposure risks.
Introduction
Exposure of pregnant women to ionizing radiation during radiological procedures might unintentionally happen in the early months of pregnancy. The hazards from radiation exposure threaten the intact development of the fetus and disturb the rest of family. After radiation exposure, several types of complications and disorders may be manifested latterly like intrauterine growth restriction, prenatal or neonatal death, congenital malformations, and mental retardation.In the same framework, radiation dose assessment of embryo/fetal has increasingly gained a great concern in nuclear medicine practices through dose computation and risk estimation. In common practice, different types of radioisotopes and wide range of radioactivity are utilized for diagnostic and therapeutic purposes that might exceed the tolerated fetus dose. Hence, developing precise methods to precisely benchmark radiation dose to embryo/fetus are of great importance with respect to the radiation protection legislations. These models should inherently take into account the transfer of radionuclides across the placenta, distribution and retention of the radionuclides in embryonal/fetal tissues, growth of the embryo/fetal, and photon irradiation sources in the placenta and maternal blood.[1]
In general, prenatal radiation exposure of approximately 10 mGy might enhance the risk of fetal disorders such as prenatal death, microcephaly, reduced intelligence quotient, organ malformation, mental retardation, intrauterine growth retardation, and childhood cancers. However, it was reported that radiation dose <50 mSv (5 rem) is not associated with fetal anomalies emergence or pregnancy loss.[2] Several local and global radiation protection organizations such as the International Commission on Radiological Protection (ICRP) and the National Council on Radiation Protection and Measurements declared that fetal radiation doses below 100 mGy should not be used as justification for terminating pregnancy.[3] According to the American College of Obstetricians and Gynecologists, potential health risks may arise after cumulative radiation exposure exceeding 50 mSv, depending on the dose and stage of pregnancy.[2]
Since, many radiopharmaceutical agents are in use for the nuclear investigations, the variation in radionuclides biokinetics and excretion rate is impossible to consider within the fetal dose estimation process.[4] However, practical vehicles have been developed for estimating the radiation dose from both internal radiation emitters and CT.
This study was dedicated to calculate fetal absorbed dose in pregnant women subjected to SPECT scan with 99mTc-labeled radiopharmaceuticals. A further goal was to compare the fetus dose values generated from the mentioned procedures with the risk thresholds reported by ICRP 84.
Methods
A group of pregnant female patients applied to receive a consultation from the teratologic counseling center. In Turkey, Genetic Research and Diagnosis Center (GETAM) at Istanbul University-Cerrahpasa, Cerrahpasa Faculty of Medicine provides full counseling services to pregnant patients coming from all hospitals over Turkey. Through that, the pregnant women were referred to the medical physics department to estimate the fetal radiation doses.Between June 2015 and June 2021, embryo/fetal doses of 74 pregnant women underwent SPECT scans were calculated retrospectively. Gestational age was obtained from patients" specific ultrasound data. Accordingly, 68 (92%) women were in the first trimester of pregnancy and 6 (8%) were in the second trimester of pregnancy.
All pregnant women were asked to bring the essential documents that contain detailed information about the type of procedure. OLINDA/EXM 1.0 software was used to calculate embryo/fetal dose according to the following MIRD schema:

where D is absorbed dose in a target organ (mGy),
à is cumulated activity in a source organ (MBq • h), A0
is administered activity (MBq), 𝜏 is residence time (h),
S is dose factor provided in the program 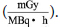
Individual embryonal/fetal dosimetry is not applicable, as no pre-imaging procedures could be tried for specific dosimetry. Attempt was made to use fetus kinetic data generated from phantom study reported by Russell et al.[5] The early 3-month and 6-month pregnant female model was selected for all calculations and only patients weight was replaced in the program.
A set of equations was used to estimate the CT related dose following SPECT/CT examinations. The calculated dose values from CT were added to that obtained from SPECT and given as a total SPECT/CT embryo/fetal dose in the results section. FetDose V4 computer software was used to compute the fetal absorbed dose.[6,7]
The fetal dose (Df) from CT scans was calculated using the formula (2) as seen below:
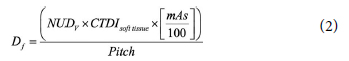
where CTDI is CT dose index and CTDIsoft tissue (mGy/100 mAs) is the CTDIair to the ICRU muscle (CTDIsoft tissue=CTDIair x 1.07) used as approximations for the dose to soft tissue within the body and NUDV is the sum of the normalized doses for all 5 mm slabs lying within the scan volume.[2,6]
Results
The distribution of the fetuses in relation to the gestational age of the subjects was shown in Figure 1. About 68 pregnant women among the participants were majorly in the first trimester of pregnancy. The calculated fetal doses for 74 pregnant women undergone nuclear procedures were given in Table 1. 99mTc-MIBI MPS involving two distinct modes (stress and rest imaging) yielded the highest mean embrio/fetal dose as (8.88+5.55=14.43 mGy) compared to other nuclear medicine procedures. A slight increase in the fetal dose up to 15.63 mGy was observed in MPS SPECT/CT depending on the CT dose contribution. Whereas, 99mTc- DMSA static renal scintigraphy recorded the lowest embryo/fetal dose among the other diagnostic procedures (mean 1.06 mGy). The average embryo/fetal dose values for 13 pregnant women underwent bone scintigraphy with 99mTc-MDP were about 5 mGy (range: 3.76? 4.70 mGy). In addition, SPECT/CT over abdomen and pelvis led to extra 8 mGy absorbed dose making the total embryo/fetal dose in MDP 12.07 mGy. The most common scintigraphy is thyroid scintigraphy where the embryo/fetal dose range of 35 pregnant patients was 1.86?4.07 mGy with an average of 3.13 mGy. Overall, the participant subjects were categorized according to the absorbed dose intervals as exhibited in Figure 2.Table 1 Embryo/fetal doses from nuclear medicine diagnostic examinations
Fig. 1. Number of fetuses during pregnancy.
Fig. 2. Distribution of embryo/fetal doses according to the number of fetuses
Discussion
Diagnostic and therapeutic nuclear medicine examinations are usually conducted using different radiopharmaceuticals with variable bio-kinetics. To date, 99mTc is heavily used in the scintigraphy of the main organs like thyroid, lung, liver, kidney, and bone. Pregnant women might unintentionally undergo radiation procedures in the daily practice. The stream of the present study was to quantify and explore the level of radiation dose to the fetus from different kinds of radiopharmaceutical examinations. According to the previous studies, the maternal bladder is the deemed the main source of fetus radiation dose.[8-10] The average fetal from 99mTc-MDP was 4.41 mGy (range: 3.76-5.64 mGy). The embryo/fetal dose was increased to 12 mGy twice the dose from SPECT when SPEC/CT was acquired. In addition, the corresponding radiation dose due to MPS is relatively higher compared to other scintigraphy procedures ranging from 8.88 to 14.43 mGy, taking into account the large amount of activities (e.g., 740+370 MBq for stress and rest imaging). Likewise, it was reported that the fetal dose of a patient administered by 1000 MBq 99mTc-MIBI is 12 mGy.[11] With adding the CT dose portion, the overall embryo/fetal dose reaches 15.63 mGy which is the highest value among other 99mTc radiopharmaceuticals.In contrast, 99mTc-diethylene triamine pentaacetic acid (DTPA) is rapidly distributed throughout the extracellular fluid space following intravenous injection, while the most of the activity accumulates in the kidneys and excreted out through the urinary bladder. The average dose of embryo/fetal for three pregnant women underwent dynamic renal scintigraphy with 99mTc-DTPA was 2.48 mGy. In another study, fetal dose values for 99mTc-DTPA scan were calculated as 1.66 mGy for <3 months of pregnancy.[12] Moreover, 35 patients subjected to thyroid scintigraphy with 185-370 MBq 99mTc-pertechnetate. The respective fetal dose was 3.13 mGy at 2?21 weeks of gestation. Similarly, embryo/fetal dose was given as 0.8 mGy after administration of 75 MBq 99mTc-pertechnetate.[13]
On the other hand, ICRP Publication 84 stated that radiation-induced malformation has a threshold of 50-100 mGy (5-10 rad). A serious fetal damage might occur when embriyo/fetal doses exceed 500 mGy (50 rad) taking into consideration the radiation type and stage of pregnancy.[3]
Eventually, the diagnostic nuclear medicine examinations often induce fetal dose less than the pregnancy terminating dose threshold (100 mGy) reported by ICRP 84. To be remembered, radiation exposure may develop deterministic and stochastic effects on the fetus. The deterministic effects are dose-correlated and lead to distinct damage or mutations in the fetus DNA genes. However, the stochastic effect has no dose threshold ensuring possible side effects even with small doses.[2] Furthermore, the carcinogenesis risk has a linear correlation and monotonic increase with the radiation dose, and therefore exposure to low dose levels may boost the cancer occurrence risk.[14] Overall, adequate maternal hydration and frequent urination reduce fetal exposure to radionuclides, however, longterm watching after birth still an essential to unveil the stochastic effects after radiation exposure.
To this end, 99mTc-labelled agents are short lived radiopharmaceuticals and fetal dose exceeding 100 mGy from a single procedure is impossible. Thus, teratogenic consultation is distinctly recommended and medical aborts decision can be made in cooperation with family, obstetrician, and medical physicist.
Conclusion
It was determined that embryo/fetal doses increased with the introduction of SPECT/CT into nuclear medicine applications. The embryo/fetal radiosensitivity is extremely high and therefore questioning women of childbearing age before scintigraphy should be the first-line strategy to avoid radiation exposure toxicities.Peer-review: Externally peer-reviewed.
Conflict of Interest: All authors declared no conflict of interest.
Ethics Committee Approval: The study was approved by the İstanbul University Cerrahpaşa Faculty of Medicine Ethics Committee (No: 219488, Date: 09/07/2015).
Financial Support: None declared.
Authorship contributions: Concept - N.İ.I., M.D.; Design - N.İ.I.; Supervision - N.İ.I., M.D.; Funding - M.D., N.İ.I.; Data collection and/or processing - M.D., N.İ.I.; Data analysis and/or interpretation - M.D., N.İ.I; Literature search - M.D., N.İ.I; Writing - N.İ.I.; Critical review - M.D.
References
1) ICRP Publication 88. International Commission on
Radiological Protection. Doses to the embryo and fetus
from intakes of radionuclides by the mother. Ann
ICRP 2001;31.
2) ACOG Committee on Obstetric Practice. ACOG
Committee opinion. Number 299, September 2004
(replaces No. 158, September 1995). Guidelines for
diagnostic imaging during pregnancy. Obstet Gynecol
2004;104(3):647-51.
3) ICRP Publication 84. International Commission on
Radiological Protection. Pregnancy and medical radiation.
Ann ICRP 2000;30.
4) ICRP Publication 106. International Commission on
Radiological Protection. Radiation dose to patients
from radiopharmaceuticals. Ann ICRP 2008;38:1-2.
5) Russell J R, Stabin M, Sparks RB, Watson E. Radiation
absorbed dose to the embryo/fetus from radiopharmaceuticals.
Health Physics 1997;73(5):756-69.
6) Ozbayrak M, Cavdar I, Seven M, Uslu Besli L, Yeyin N, Tanyildizi H, et al. Determining and managing fetal
radiation dose from diagnostic radiology procedures
in Turkey. Korean J Radiol 2015;16(6):1276-82.
7) Osei EK, Kotre CJ. Equivalent dose to the fetus from
occupational exposure of pregnant staff in diagnostic
radiology. Br J Radiol 2001;74(883):629-37.
8) ICRP Publication 60. International Commission on
Radiological Protection. 1990 recommendations of
the ICRP. Ann ICRP 1991;21.
9) McKenzie AF, Budd RS, Yang C, Shapiro B, Hicks RJ.
Technetium-99m-methylene diphosphonate uptake
in the fetal skeleton at 30 weeks gestation. J Nuc Med
1994;35(8):1338-34.
10) Hedrick WR, Simone RN, Wolf BH, Langer A. Absorbed
dose to the fetus during bone scintigraphy. Radiolog
1988;168(1):245-54.
11) Stabin MG. Radiation dose and risks to fetus from
nuclear medicine procedures Physica Medica
2017;43:190-8.
12) Arteaga MV, Carrillo HV, Benites CR, Rengifo KM,
Garcia AJ, Gomez AR. Absorbed dose in the uterine
wall and fetus by 99mTc administration (DTPA, DMSA
and MAG3. Momento 2021;62:32-42.





